April is Stress Awareness Month, a time dedicated to recognizing how stress affects our physical and mental health. While many people associate stress with headaches, fatigue, or anxiety, fewer realize that skin is one of the organs most affected by chronic stress. As the body’s largest organ and a highly responsive interface with the external environment, skin often reflects internal physiological changes triggered by stress.
Dermatologists and researchers increasingly recognize the “brain–skin connection,” a complex interaction between the nervous system, endocrine system, and immune response that influences skin health. When stress becomes chronic, it can disrupt the skin’s protective barrier, worsen inflammatory skin conditions, accelerate aging, and impair healing.
Understanding how stress impacts the skin can empower patients to take steps that protect both their overall health and their skin health.
The Brain–Skin Connection
The link between stress and skin health is rooted in the body’s stress response system, known as the hypothalamic-pituitary-adrenal (HPA) axis. When the brain perceives stress, the HPA axis releases hormones including cortisol, adrenaline, and other mediators that help the body respond to perceived threats.
While this response is helpful in short bursts, chronic stress keeps these hormones elevated, which can negatively affect multiple organ systems, including the skin. Research shows that stress hormones can influence skin immune function, inflammation, and barrier integrity.
Importantly, the skin itself contains receptors for stress hormones and can even produce stress-related mediators locally. These interactions create a two-way communication pathway between the brain and the skin, meaning emotional stress can directly influence skin biology.
How Stress Disrupts the Skin Barrier
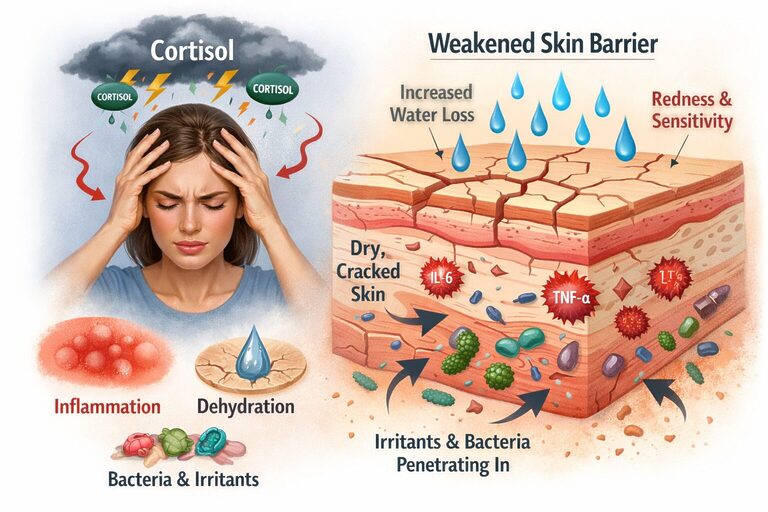
One of the most significant ways stress impacts the skin is by weakening the skin barrier. The skin barrier is the outermost layer of the epidermis that protects against bacteria, allergens, and environmental irritants while retaining moisture.
Studies show that stress-induced cortisol reduces essential lipids and structural proteins in the epidermis. These lipids are critical for maintaining hydration and barrier strength. When cortisol levels rise, the skin may experience decreased hydration and increased transepidermal water loss, meaning moisture escapes more easily.
Research also demonstrates that psychological stress can delay the recovery of the skin barrier after injury or irritation. Stress triggers inflammatory molecules such as interleukins and tumor necrosis factor-alpha, which can disrupt normal skin repair mechanisms.
Clinically, patients may notice symptoms such as increased dryness or dehydration, skin sensitivity, redness or irritation, or the worsening of existing skin conditions
A compromised barrier can also make skin more susceptible to environmental triggers and infections.
Stress and Acne
Acne is one of the most well-known skin conditions affected by stress. While stress alone does not directly cause acne in every individual, research consistently shows that stress can worsen acne severity in people who are already prone to breakouts.
Stress hormones stimulate sebaceous glands to produce more oil (sebum), creating an environment where acne-causing bacteria can thrive. Cortisol has been shown to increase sebaceous gland activity and lipid production, which contributes to acne development.
Multiple studies have found a statistically significant correlation between stress levels and acne severity. For example, research examining acne in female students demonstrated that higher perceived stress scores were associated with more severe acne.
Additionally, stress may slow the healing process of acne lesions. Research indicates that psychological stress can delay wound healing by as much as 40 percent, meaning blemishes may take longer to resolve.

Stress and Inflammatory Skin Conditions
Stress does not only affect acne. It can also trigger or worsen inflammatory skin diseases, including:
- Psoriasis
- Eczema (atopic dermatitis)
- Rosacea
- Chronic urticaria (hives)
Stress activates immune pathways and inflammatory mediators in the body. These immune responses can increase itching, redness, and inflammation in susceptible individuals.
For patients with eczema or psoriasis, stress can create a frustrating cycle. Skin flare-ups increase emotional distress, which in turn worsens the underlying skin condition. This cycle highlights the importance of addressing both physical and psychological components of dermatologic disease.
Stress and Skin Aging
Another important effect of chronic stress is accelerated skin aging. Elevated stress hormones contribute to oxidative stress and reduce antioxidant activity in the skin. These changes can impair collagen production and damage cellular structures responsible for maintaining healthy skin.
Clinical studies have shown that individuals experiencing moderate psychological stress demonstrated reduced antioxidant potential and increased signs of skin aging, including changes in skin texture and fine lines.
Over time, stress can contribute to:
- Collagen breakdown
- Reduced skin elasticity
- Fine lines and wrinkles
- Dull or uneven skin tone
Because collagen and extracellular matrix proteins are essential for skin structure, their disruption can accelerate visible aging.
Stress Slows Skin Healing
Stress can also impair the skin’s ability to repair itself after injury. Normal wound healing requires coordinated immune activity, collagen synthesis, and cell regeneration. Chronic stress disrupts these processes by altering immune responses and inflammatory signaling.
Researchers have observed that stress hormones and inflammatory mediators can delay wound healing and impair tissue repair, which can affect everything from acne lesions to surgical recovery.
For patients undergoing dermatologic procedures, reducing stress and supporting overall wellness may contribute to optimal healing outcomes.
Other Skin Symptoms Linked to Stress
Because stress affects multiple biological pathways, it can lead to a variety of skin symptoms. Patients experiencing chronic stress may notice:
- Increased breakouts or oil production
- Dryness or skin sensitivity
- Flare-ups of eczema or psoriasis
- Increased itching or inflammation
- Delayed healing of cuts or blemishes
- Premature signs of aging
These symptoms highlight how closely the skin is tied to overall health and wellness.
Strategies to Protect Your Skin During Stressful Times
While stress is a natural part of life, managing stress effectively can benefit both your overall health and your skin.
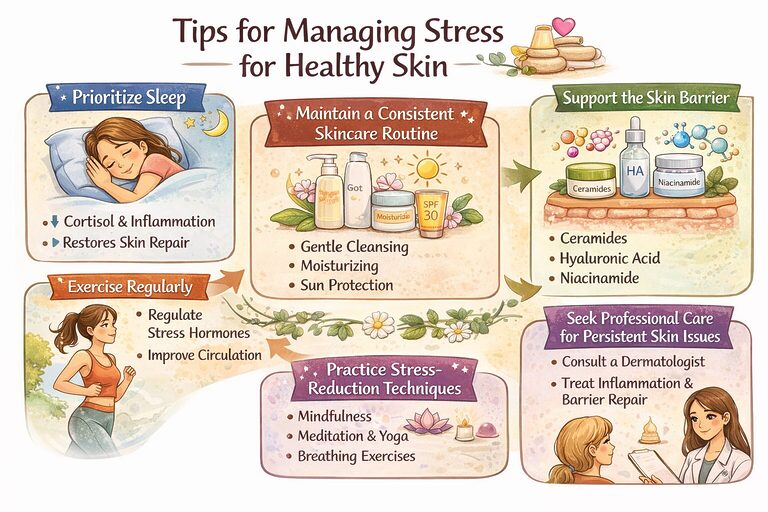
Prioritize sleep
Poor sleep increases cortisol levels and can worsen inflammation in the body. Consistent, restorative sleep supports skin repair and regeneration.
Maintain a consistent skincare routine
Gentle cleansing, moisturizing, and sun protection help reinforce the skin barrier, particularly during periods of stress.
Support the skin barrier
Products containing ceramides, hyaluronic acid, and niacinamide can help restore hydration and strengthen the skin barrier.
Exercise regularly
Physical activity helps regulate stress hormones and improves circulation, which supports skin health.
Practice stress-reduction techniques
Mindfulness, meditation, yoga, and breathing exercises can reduce activation of the stress response and improve overall well-being.
Seek professional care for persistent skin issues
If stress is worsening a skin condition such as acne, eczema, or psoriasis, a dermatologist can recommend treatments that address both inflammation and barrier repair.
When to See a Dermatologist
Occasional stress-related breakouts or irritation are common, but persistent or worsening symptoms should be evaluated by a dermatologist. Professional evaluation can help identify underlying conditions and provide targeted treatments that support healthy skin.
Dermatologic treatments may include prescription medications, barrier-repair therapies, and individualized skincare recommendations.
Supporting Skin Health During Stress Awareness Month
Stress Awareness Month serves as an important reminder that mental and physical health are deeply connected. The skin often reflects what is happening inside the body, making it one of the most visible indicators of chronic stress.
By recognizing the relationship between stress and skin health, patients can take proactive steps to support both their emotional well-being and their skin. Healthy lifestyle habits, stress management techniques, and appropriate dermatologic care can help maintain healthy, resilient skin—even during life’s most stressful moments.
If you are experiencing stress-related skin concerns, our dermatology team is here to help. Together, we can develop a personalized treatment plan that supports your skin and your overall health.
